News & Updates
You will need to eat a soft diet for around six weeks after jaw surgery.
If you have a broken or fractured jaw, you will know that it can be very painful. A broken jaw can occur when one or more of the joints that connect the skull and the lower jawbone are injured. Some of the most common causes of this type of injury include trauma caused by car accidents or assault; sports injuries; and falls. Unfortunately, a broken jaw can make it difficult to eat — read on to find out about the type of diet that is best during your recovery period, and how you can manage any discomfort that you feel…
What does a broken jaw feel like?
A broken jaw generally feels quite painful. Other common symptoms include swelling of the jaw and face; bleeding; discomfort when biting and chewing; stiffness of the jaw; bruising of the jaw and face; and dental-related issues, such as loose teeth and sore gums. In some cases, it is possible to experience breathing difficulties as a result of a jaw injury.
What can you eat with a broken jaw?
Because you are likely to experience discomfort when eating, as well as pain and stiffness in the jaw, it is advisable that you eat a soft diet while you recover from a broken jaw. It is best to avoid crunchy and chewy foods completely during this time — these types of foods can place excess strain on your jaw and cause further pain. Rather choose foods that don’t require much chewing — some good examples include soup; soft fruits; pasta; yoghurt and oatmeal.
If you have to have your jaw wired, you won’t be able to open and close your mouth for much of your recovery period. For this reason, you will need to get your daily nutrients through a straw. In this case, pureed fruits and vegetables, as well as smoothies and soups are all good options.
While your broken jaw heals, be sure to avoid hot foods and drinks as you may experience heightened sensitivity during this time. Eat your food at a lukewarm temperature so as to avoid irritation in the mouth.
What are the treatment options?
Fortunately, there are a number of ways in which broken and fractured jaws can be effectively managed and repaired. In fact, surgery for this type of injury usually leads to complete recovery.
If you are referred for surgery to repair a broken jaw, your surgeon will administer a general anaesthetic. They will then make an incision inside your mouth in order to access the site of the fracture or break. The broken jawbone is then put back together and held in place with the help of small plates and screws. When your surgeon has completed the jaw reconstruction, they will close the incision with dissolvable stitches.
In some cases, your surgeon may place elastic bands in order to guide the jaw into the correct position after surgery. These elastics are attached with the use of temporary metals or braces.
After surgery, you can expect some discomfort and swelling at and around the site of surgery. Your surgeon will prescribe the appropriate medications to ease your pain. They will also explain how to keep your surgical wounds clean and free from infection.
How can OMFS help?
At OMFS, we offer a number of procedures for facial trauma, including treatments for broken and fractured jaws. If you have been referred for jaw surgery, we encourage you to get in touch with us to discuss your treatment options in detail. Our team will also let you know what to expect from the recovery process, and how to best manage any post-surgical pain that you experience.
If you would like to find out more about surgery for a broken jaw and what it involves, please have a look here.
To arrange an appointment, please get in touch here or give us a call on (03) 9347 3788. Our team is highly experienced and committed to providing you with top-quality care.
Obstructive sleep apnoea can have a serious impact on one’s general health.
Obstructive sleep apnoea is a condition that occurs when the airway is restricted in some way. As a result of this restriction, the body does not receive enough air during sleep — this leads to pauses in breathing throughout the night. If left untreated, the condition can lead to a number of other health concerns, as well as some uncomfortable symptoms. Read on to find out more about obstructive sleep apnoea and how it can be managed…
What are the symptoms?
One of the most common symptoms of obstructive sleep apnoea is loud snoring. Other possible symptoms include daytime fatigue, restless sleep, regular waking throughout the night, and teeth grinding. If you suffer from obstructive sleep apnoea, you may also wake up with a headache and/or a sore jaw on a regular basis.
If left untreated, the condition can increase one’s risk of developing a number of other health problems. These include high blood pressure; stroke; heart-related problems like heart failure and irregular heartbeats; diabetes; depression; anxiety; and chronic headaches. Daytime sleepiness can also contribute to poor performance at work or school, and can interfere with day-to-day activities, as well as one’s overall sense of wellbeing.
How can it be managed?
Fortunately, there are a number of ways in which obstructive sleep apnoea can be managed. In some cases, certain lifestyle changes can be enough to resolve the symptoms of the condition — these may include weight loss; more regular exercise; limiting one’s consumption of alcohol; smoking cessation; changes in sleep positions; and limiting one’s use of sedative medications.
If lifestyle changes do not alleviate the symptoms of the condition, the use of an oral appliance may be recommended. Oral appliances are designed to keep the throat and airway open, and are often suitable in cases of mild to moderate obstructive sleep apnoea. Some patients may benefit from continuous positive airway pressure (CPAP), which is a treatment that involves the use of a machine that fits over the nose during sleep. The machine delivers air pressure, which helps to reduce respiratory disruptions throughout the night.
If non-surgical treatments prove unsuccessful, you may be referred for surgery. There are a number of surgical procedures available, all of which help to alleviate the symptoms of obstructive sleep apnoea and reduce the risk of other health issues. Surgery may be performed in order to expand the jaws, or excess tissue of the soft palate may be surgically removed in order to resolve airway restriction. The surgical method that is most appropriate for you will depend on the severity of your symptoms, as well as your particular concerns.
How can we help?
If you are suffering from any of the symptoms of obstructive sleep apnoea, such as daytime fatigue, restless sleep, or loud snoring, we encourage you to come in and see us for a consultation.
At OMFS, we offer a number of treatments for the condition, including some surgical options. If you are a suitable candidate for surgery, your surgeon will let you know which method is best for you and will discuss the relevant procedure in detail with you. Your surgeon is also available to address any questions or concerns that you have regarding your treatment so that you are properly informed before you go ahead with treatment.
If you would like to find out more about our procedures for obstructive sleep apnoea, please have a look here.
To arrange an appointment, please get in touch here or give us a call on (03) 9347 3788. Our team of surgeons is highly qualified and experienced, and works hard to provide top-quality care to each and every patient.
Besides the management of obstructive sleep apnoea, we also offer a range of other oral and maxillofacial procedures, including oral surgery, implants and grafting, jaw surgery and TMJ management. To see the full scope of our services or to learn about a specific procedure, please have a look here.
Dental implant failure is rare, but it can happen.
Dental implants are, usually, very successful procedures that bring a long-term boost to oral health. However, in a small number (about 5%) of cases, a dental implant may fail.
Read on to learn more about dental implants, including how to minimise the risk of early and late dental implant failure.
What is a dental implant?
A dental implant is a safe, effective treatment usually undertaken to replace a missing tooth. It is considered an ideal solution for restoring oral form and function, suitable for patients who have good general oral health, but not for those who have lost a tooth due to injury or gum disease.
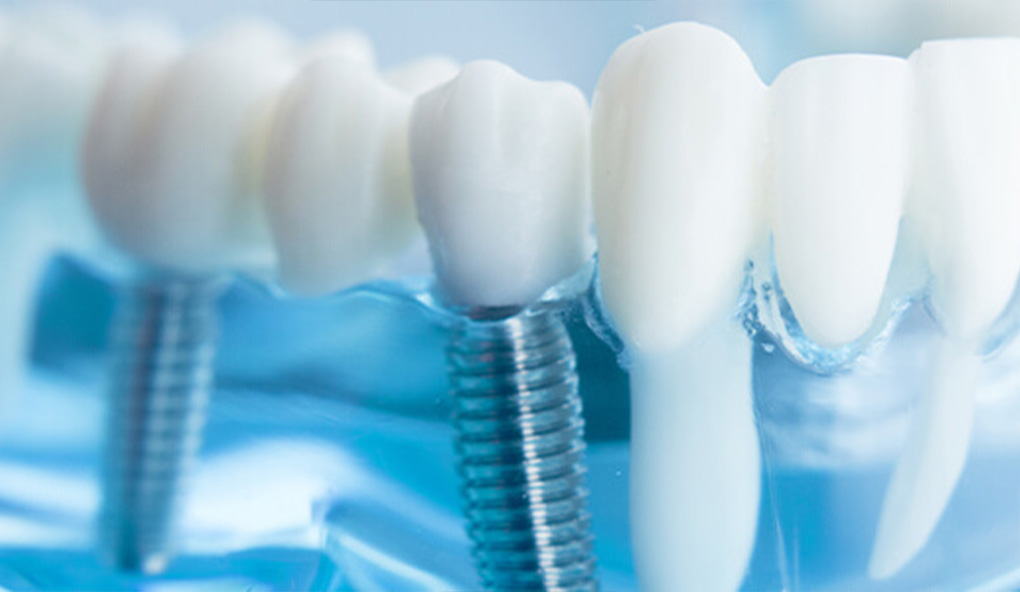
Dental implants are usually made of three parts: a titanium implant that is inserted into the jaw bone; an attachment, called an abutment, that is connected to the implant; and a crown at the top, which is aligned and matched to the shade of your existing teeth.
Why can dental implants fail?
There are two main reasons why, in a small percentage of cases, dental implants may fail.
Peri-implantitis is a form of gum disease where the mouth becomes infected, and this infection damages the bone around the implant. Its cause is usually poor oral hygiene (inadequate brushing and flossing).
On the other hand, failed osseointegration is when your jaw bone is unable to grow around the dental implant to make it secure. Failed osseointegration may have many causes, including the structure and strength of your bones, whether or not you are a smoker, the technique used by your dental surgeon, and the quality of the surgery itself.
What are the causes of early dental implant failure?
Early dental implant failure risks are limited to the short-term (usually the recovery period following a dental implant procedure).
Some key contributing factors to avoid include deprived blood supply to the implant area, the development of infections in the mouth, and moving or shifting of the implant during the healing phase.
This is why it is vitally important to follow the directions of your dentist immediately following a dental implant procedure. You will need to make some short-term lifestyle adjustments — such as quitting smoking, avoid certain medications, and making dietary changes — in order to avoid long-term problems.
What are the causes of late dental implant failure?
It is even less common — but not impossible — for dental implants to fail after a number of successful years. These longer-term causes of dental implant failure are usually related to natural wear and tear of the body (such as weak bones or unhealthy gum tissue), but good oral hygiene can reduce the risk of dental implant failure.
Some key causes of late dental implant failure include bacterial infections (sometimes caused by impacted food) and generally poor oral hygiene, which can lead to gum diseases. It is also important not to put excessive stress on the implants (consult your dentist if you grind your teeth at night), and it is recommended that you avoid repeated exposure of your head and neck areas to radiation.
What dental implant precautions can be taken?
Before your dental implant placement, have a detailed discussion with your dentist about any risk factors that can limit the success of your procedure. Understand the different lifestyle and dietary adjustments that you are committing to before proceeding.
Ensure that you elect a skilled, qualified dental surgeon to perform your dental implant procedure — not all surgeons are equal, and any risk of dental implant failure will be minimised by working with a trusted professional.
How can we help?
At Oral and Maxillofacial Surgeons (OMFS), our surgeons are recognised as some of the best in their respective fields, with associations and affiliations to the leading teaching hospitals in the country. Dental implants have become an important part of modern dentistry, and we offer expert procedures with long-lasting successful results. For more about dental implants, please read more here.
No matter what your diagnosis is, all our patients at OMFS are treated with respect and dignity. To arrange an appointment to meet our passionate team and to discuss your treatment options, please get in touch here.
In addition to a comprehensive range of oral and maxillofacial surgery treatments, our services include consultations and second opinions, medico-legal reporting, local anaesthetic procedures in a comfortable office environment, and general anaesthetic procedures in various hospitals throughout Melbourne and regional Victoria. To find out more about all we have on offer, please consult our website
Genioplasty, or chin augmentation, is performed to reposition and recontour the chin.
Chin augmentation, also known as genioplasty, is a kind of surgery that is performed on the chin. The purpose of the procedure is to recontour and reposition the chin for a more pleasing aesthetic. In most cases, the surgery is performed for cosmetic reasons and is an ideal option for those who are dissatisfied with the appearance of their side jawline profile. Read on to find out more about the procedure, how it works, and what you can expect from the recovery process…
What does the surgery involve?
There are a number of ways in which genioplasty may be performed. How your treatment is conducted will depend on your particular concerns and aesthetic goals. In some cases, the chin is pushed forward, while in other cases, it is moved backwards. The procedure can also be performed to make vertical changes, in which case the chin will be made longer or shorter. The chin can also be moved from side-to-side, which can help to improve symmetry.
When it comes to the procedure itself, there are two main types of surgery: sliding genioplasty and chin implant surgery. In the case of a sliding genioplasty, your surgeon will make an incision inside the mouth and cut and reposition the chin bone. The bone will then be secured in its new position with small plates and screws. This technique is often used to correct a condition known as retrogenia, in which the chin is too far back in relation to the rest of the face.
In the case of chin implants, your surgeon will place some biocompatible plastic into the chin. This material will integrate with the bone over time. Chin implants are often a good option for those who would like to enlarge or push forward their chin.
How long does recovery take?
Although genioplasty is not generally considered a painful procedure, you are likely to experience some discomfort in the days following surgery. Your surgeon will recommend some pain medication to alleviate any uncomfortable side effects. You may also be prescribed antibiotics in order to reduce the risk of infection.
It is also completely normal to experience some swelling, redness and bruising after surgery. These side effects should, however, resolve in time. Swelling can be minimised with the use of a cold compress. It can also be helpful to sleep upright in the first few days of recovery.
Most patients are able to remove their wound dressings within around five days following surgery. It is advisable to avoid exercise for around 10 days following surgery, and contact sports for six to eight weeks.
How can we help?
At OMFS, we offer chin augmentation for patients who would like to improve the appearance of their chin and jawline. In some cases, we perform the procedure at the same time as corrective jaw surgery in order to improve facial symmetry, as well as the overall appearance of the facial features. If you are unhappy with the appearance of your jaw and your side jaw profile, we encourage you to come in and see us for a consultation. We will let you know if the treatment is right for you and explain the details of the procedure. If you would like to find out more about chin augmentation and what the process involves, please have a look here for some more information.
To arrange an appointment to meet our passionate team and to discuss your treatment options, please get in touch here. We offer a comprehensive range of procedures — to see our full range of services, please have a look here. Whether you require a surgical intervention for an existing concern, or you need an emergency procedure to resolve a facial trauma, we can help.
Oral medicine is a speciality of dentistry that focuses on the diagnosis and management of conditions that affect the maxillofacial region.
If you are suffering from a condition that affects the oral and maxillofacial region, you could likely benefit from seeing an oral medicine specialist. Oral medicine specialists are required to complete advanced and specialised training, which allows them to diagnose and manage a wide range of issues. Read on to find out what an oral medicine specialist does, and what kinds of concerns they can help resolve…
What training is required?
An oral medicine specialist is a dentist who has completed additional training that allows them to specialise. The additional education is advanced and allows them to take on a range of diagnostic and management approaches. Thanks to their specialised training, an oral medicine specialist qualifies with considerable knowledge of many medical conditions that affect the orofacial region. They can use highly specialised techniques and can often diagnose and manage oral pathologies, disorders and diseases that require specialist skills and knowledge.
What does an oral medicine specialist do?
An oral medicine specialist is a doctor who has been through specialised training that allows them to diagnose and manage a range of disorders related to the orofacial area. An oral medicine specialist is qualified to address a wide range of oral mucosal abnormalities, such as ulcers, growths, cancers, infections and allergies; disorders related to the salivary glands; temporomandibular disorders; taste and smell disorders; and oral manifestations of systemic and infectious diseases.
As part of their services, an oral medicine specialist is qualified to perform a comprehensive range of procedures to diagnose and treat various conditions. These include biopsies; imaging studies like x-rays, CT scans and MRIs; salivary and blood tests; medical management; and specialised injections, such as in the case of TMJ and associated jaw and facial pain.
An oral medicine specialist is also able to perform various dental procedures, and may even work with other healthcare practitioners, including general practitioners, dentists, oncologists and maxillofacial surgeons to formulate a treatment plan.
When should you see an oral medicine specialist?
You may be referred to an oral medicine specialist by your dentist or doctor, especially if you have a concern related to the soft tissues of your mouth. You may benefit from seeing an oral medicine specialist if you suffer from frequent or very painful mouth ulcers; general oral pain; or a dermatological condition that is affecting your mouth. You may also be referred to an oral medicine specialist if your doctor or dentist has recommended a biopsy of your mouth to check for cancer.
Other reasons for consulting with an oral medicine specialist include oral candidiasis; oral dysplasia; and geographic tongue, all of which may present with red and white patches in the mouth. Skin diseases that often have oral manifestations, and which can be diagnosed and managed by an oral medicine specialist include certain allergic reactions; lichen planus, which is an inflammatory skin condition; and lupus erythematosus, an autoimmune disease.
How can we help?
At OMFS, our oral specialist medicine specialist Dr Katrusha Hull is available to assist in the diagnosis and management of a range of issues. She has a particular interest in oral mucosal diseases, potentially malignant oral lesions, and orofacial pain conditions including burning mouth syndrome. Dr Hull has completed extensive training in the field and was awarded a PhD in 2018 for her research into the underlying mechanisms of graft-versus-host disease following stem cell transplantation.
A key member of the OMFS team, Dr Hull also holds specialist positions at the Peter MacCallum Cancer Centre, Monash Medical Centre and the Royal Dental Hospital of Melbourne. If you would like to find out more about Dr Hull, her qualifications and areas of expertise, please have a look here.
To arrange a consultation to see Dr Hull or any of our other specialists, please get in touch here or give us a call on (03) 9347 3788.
Dental bone grafts are performed in order to increase the amount of bone in the jaw or to improve support for an implant.
If you need a dental implant, it is possible that you may require a bone graft to ensure the success of the procedure. Without enough bone and soft tissue in the jaw and around the implant site, you may not be able to have dental implants placed. The bone grafting procedure helps to increase the amount of bone in an area of the jaw where bone has been lost. Read on to find out how the procedure works…
What is a bone graft?
A dental bone graft involves the harvesting of bone from other areas of the patient’s body (commonly from other areas of the jaw) and attaching it to the bone material in the jaw. In some cases, the patient’s own bone may be used together with other grafting materials in order to reduce additional deterioration. In complex and severe cases, bone may be harvested from other areas of the body, such as the hip.
Depending on the severity of your bone deterioration, the bone grafting procedure may be performed either under local or general anaesthetic. Your surgeon will make an incision in your gum and separate the bone from the area in which the graft will be placed. The bone material will then be placed between two areas of bone that will grow together over time. The bone graft will be secured in place with special surgical screws, or a dissolvable material. Your surgeon will then stitch the incision closed.
When is a bone graft recommended?
There are a number of reasons one might undergo a bone graft procedure. One of the most common situations in which the procedure is performed is when a patient needs a dental implant but has insufficient bone and soft tissue to support the restoration. Bone grafting helps to create a strong foundation for an implant and increases the chances of long-term implant success. A bone graft may also be necessary in the case of tooth loss or severe gum disease where bone loss is an issue. If you experience bone loss in the jaw, your nearby teeth and gum tissue can be affected, and a bone graft can help to stabilise the area and prevent further bone loss from occurring.
A bone graft can also be helpful for patients who have lost significant bone loss in the jaw, and who have noticed a change in their appearance as a result. A loss of bone mass in the jaw can cause the skin around the jaw to appear more wrinkled than before, while the lower jaw may appear to protrude.
What does the recovery involve?
Once your bone grafting procedure is complete, your surgeon will let you know how best to take care of the site of surgery. You may experience some pain and discomfort as you heal, and your surgeon will prescribe medications to help alleviate these symptoms.
You will need to eat soft foods for a few days following surgery, and it is best to avoid hot drinks as these can cause irritation in the mouth.
How can we help?
At OMFS, we offer bone and soft tissue grafting procedures, which are often completed before dental surgery. The procedures work by replacing missing bone and tissue so that implants can be successfully placed. In some cases, the grafting procedure may be completed at the same time as dental implant surgery. To find out more about our bone and soft tissue procedures at OMFS, please have a look here. If you would to make an appointment, please get in touch with us here.
Impacted wisdom teeth occur when the back molars are stuck beneath the gum or don’t have space to erupt through the gum.
If you have noticed pain and swelling of the jaw or face, or your gums are swollen and tender, it could be a sign that you have an impacted wisdom tooth. Wisdom teeth become impacted when there is not enough room for them to erupt through the gum or when the teeth get stuck under the gum. Sometimes, impacted wisdom teeth don’t cause any issues, while infection can occur in other cases. When a tooth becomes infected, it can lead to considerable pain and discomfort and a number of oral health issues. Read on to find out what causes an impacted wisdom tooth and how it can be resolved…
What causes an impacted tooth?
In most cases, wisdom teeth are impacted because of inadequate space in the jaw. A wisdom tooth can sometimes become impacted when it grows at the wrong angle.
Although impacted wisdom teeth don’t always cause symptoms, they can lead to complications such as infection, tooth decay, crowding of the surrounding teeth, cysts, gum disease and damage to nearby teeth. It can be difficult to brush and floss impacted teeth correctly, which can make it difficult to maintain proper oral hygiene.
Although it is not possible to prevent an impacted tooth, wisdom teeth are not necessary for our modern diets. If wisdom tooth impaction is causing you discomfort or oral health issues, it is advisable to have your wisdom teeth removed. Wisdom teeth removal can help to prevent a number of problems from developing and will alleviate any pain caused as a result of infection. Even if you don’t experience any symptoms, your dentist or oral surgeon may advise that you undergo wisdom teeth surgery.
How are impacted wisdom teeth resolved?
If you have been diagnosed with impacted wisdom teeth, your dentist or oral surgeon may recommend that you have them surgically removed.
During the procedure, an incision will be made in your gums through which any problematic bone and the impacted tooth will be removed. Depending on the case, the tooth may need to be removed in one piece or sectioned into smaller pieces prior to removal. The incision will be stitched closed, and gauze will be placed at the site of surgery.
What does recovery involve?
After you have been through a wisdom tooth extraction procedure, it is completely normal to experience some discomfort, swelling and bleeding around the site of surgery. Your surgeon will prescribe some medications to help manage any pain that you feel. You will need to stick to a diet of liquid and soft foods for around a week or so following surgery while your mouth heals.
How can we help?
At OMFS, we offer a number of oral surgeries, including wisdom tooth extraction. The procedure is very common and can go a long way in preventing complications and improving overall oral health. Untreated wisdom teeth can cause considerable pain and a range of other problems, including infection, tooth decay, and damage to the surrounding teeth and gums.
If you would like to make an appointment, please get in touch with us here. We specialise in oral and maxillofacial surgery. Besides wisdom teeth extraction, we also offer surgical removal of teeth, exposure of teeth, implants and grafting, and face and jaw surgery. To see the full list of procedures that we offer, please have a look here.
A Complete Guide to Dental Implants
A dental implant is a small titanium screw which acts as a natural tooth root and is used to replace a missing or damaged tooth root in the jaw bone. Dental implants are designed to match the size, shape, and colour of your other teeth and fit and function like real ones.
What are Dental Implants?
Dental implant procedures have been successfully performed for over 50 years to millions of people around the world. The procedure is very safe and a highly effective alternative to dentures or bridgework. The procedure is performed on patients who are in good health which ultimately minimises any risk from occurring.
Key Benefits of Dental Implants
Dental implants are the closest thing to a natural tooth, they best imitate the roots of teeth and allow for artificial teeth to fit comfortably. They also provide much more support than dentures and offer advantages such as:
- Natural appearance
- Less irritation
- Oral hygiene benefits
- Eating becomes easier
- Clearer speech
The Procedure
How the dental implant surgery is performed depends on the type of implant recommended by a professional. The highly specialised team of surgeons at Oral and Maxillofacial Surgery (OMFS) can point you in the right direction following a consultation.
The dental implant procedure involves a small titanium screw being drilled down into the jawbone to act like a natural root. It’s designed to fuse with the jawbone and become a permanent fixture. Once the implant has been placed into the jawbone, the bone will begin the healing process known as osseointegration. As time progresses, the bone heals and fuses to the screw to hold it in place usually over a period of 3-6 months. Once fully healed, the screw is topped with an artificial tooth or crown to restore the full function of your smile.
Evaluation Process and Stages
A typical dental implant procedure is normally spaced out over a few months, which allows for the experienced and dedicated surgeons at OMFS to ensure excellent patient care and optimal outcomes.
Following an initial consultation, the evaluation process may include:
- Dental exam with scans, x-rays, and 3D imaging
- A thorough review of your medical history and conditions
- Development of a tailored treatment plan
Summary of the Dental Implant Procedure
- You will usually be given an anaesthetic to minimise the pain during the procedure
- Removal of any damaged tooth
- Preparation of the jaw bone if needed (bone grafting, augmentation)
- Hole in the jaw bone is drilled to place implant
- Healing process where the bone grows around the implant (osseointegration)
- Once the implant is stable the abutment will be placed (connection between the screw and false tooth)
- Finally, the artificial tooth is connected onto the abutment
Post Dental Implant Procedure and Care
Despite the high level of care taken by your surgeon at OMFS, you may experience some common discomforts following the dental implant procedure which can include:
- Pain and swelling
- Bruising
- Minor bleeding
- Infection
- Gingivitis
- Nerve injury
To reduce any pain or irritation following the surgery you may require pain medication or antibiotics. After surgery, it is important to let your body rest. Drink plenty of fluids and eat soft foods such as soups, pureed foods and vegetables for the first few days. No special aftercare is required for a dental implant. Practice good oral hygiene by brushing and flossing and have regular dental check-ups.
Contact OMFS to book in for a consultation
Don’t be scared of the results, focus on the positive change which will make you smile! Each and every patient is different, and the professional team at OMFS will tailor a dental implant procedure to suit your individual needs. Get in touch today.
Dental implants restore oral function, including biting and chewing ability.
If you are missing teeth, you might be wondering what your options are when it comes to restoring oral function. One of the most effective treatments for missing teeth is the placement of dental implants — they provide stability, as well as a natural-looking appearance. But is it possible to eat all your favourite foods once you have had dental implants placed? Read on to find out what you can expect following dental implant surgery and why these restorations are well worth considering…
What are the benefits of dental implants?
Dental implants function just like natural teeth, which means that you will be able to eat any food you like once you have recovered from the procedure. In fact, dental implants are beneficial to your diet as you will be able to bite and chew with proper force. Dental implants act as permanent fixtures in the mouth, and unlike dentures, are not removable.
Besides allowing you to eat properly, dental implants also have a number of other benefits. They are aesthetically pleasing and can be coloured matched to blend in well with your remaining natural teeth. They also help to maintain bone structure and support your facial tissues as they eliminate bone atrophy caused by tooth loss.
Dental implants provide more stability than alternatives like dentures, and do not require the use of messy adhesives.
What does the procedure involve?
If you choose to have a dental implant placed, your dentist will surgically insert a bio-compatible titanium post directly into your jawbone. The post is designed to fuse with the jawbone and become a permanent fixture in your mouth. Once the implant has been placed, it will take between 3 and 6 months for it to fuse with the jawbone in a process known as osseointegration. When the site of surgery has healed and your implant has fused with the bone, your dentist will attach an abutment to the top of the implant on which a crown will be placed.
What does the recovery involve?
It takes some time to recover from dental implant surgery, so it is important to stick to a liquid diet immediately after your procedure. Once the mouth begins to heal, however, it is possible to gradually reintroduce soft foods that are easy to chew. When you have completely recovered from surgery and your implant has fused with your jawbone, your new restoration will feel just like a natural tooth and you will be able to eat a normal diet. You should enjoy improved biting and chewing function, and your implant will feel comfortable and stable in your mouth.
How can we help?
At OMFS, we offer dental implants to patients who are suffering from tooth loss and would like to restore both the appearance and function of their smile. Besides dental implants, we also offer bone and soft tissue grafting, implant-supported dentures, all-on-four implants and zygomatic dental implants. Each of these treatments provide their own unique set of benefits and we encourage you to come in for a consultation so that our team can guide you through the procedure that best suits you. If you would to make an appointment, please get in touch with us here. We look forward to welcoming you to our practice in Melbourne. Our team specialises in oral and maxillofacial surgery and operates throughout Melbourne and regional Victoria.
It’s best to stick to soft foods following oral surgery.
It is completely normal to experience some discomfort, swelling and tenderness following wisdom teeth removal. Even if you do feel some pain after your procedure, it is very important that you eat nutritious foods to aid the recovery process. By ensuring that you eat a nutritious diet, you can minimise the risk of complications following surgery; reduce side effects like swelling; and generally support healing. Read on to find out which foods are easy (and healthy) to eat after you have had your wisdom teeth removed.
Soups
Healthy vegetable soups are a great option while you are recovering from your procedure. They are packed with nutritious ingredients and are very easy to eat as they don’t require any chewing. Make sure that you choose blended soups or broths so that you don’t have to deal with chunks that could irritate your surgical wounds. Also, don’t make your soup too hot as this could also cause some irritation in the mouth — rather stick to lukewarm or cold soups while your mouth heals.
Yoghurt
Yoghurt is an excellent source of calcium and protein, plus it’s easy to eat while you recover from surgery. Opt for Greek yogurt with a smooth texture to soothe your mouth. If you feel like something different, blend some Greek yoghurt with your favourite fruit to make a nutritious smoothie. To boost your protein intake, consider adding a scoop of protein powder to your smoothie. If you do try a smoothie, it’s best to avoid using a straw — straws tend to create a suction in the mouth and can increase your risk of developing a dry socket.
Mashed vegetables and fruits
It’s best to avoid chewy and hard foods while your mouth heals, so soft, mashed fruits and vegetables are a good option. Mashed potatoes are packed with nutrients and provide plenty of energy while you are healing. Other foods that mash well include sweet potatoes, pumpkins, stewed apples, avocados and bananas.
Eggs and cheese
High in protein and easy to chew, scrambled eggs are a highly nutritious food. They’re packed with vitamins and minerals, and are also available in omega-3-enriched varieties, which can be helpful when it comes to healing. Another high-protein food, cottage cheese makes a great snack post-surgery. It has a soft texture and is very easy to chew while you recover from your procedure. Mix it into your scrambled eggs, or enjoy it on its own.
Soft fish
If you’re looking for a protein-rich meal that’s easy to eat, cooked salmon is a good choice. The fish is typically very soft, so it shouldn’t cause any discomfort to your site of surgery. Also, it’s full of healthy fats that may help to decrease inflammation and speed up the healing process.
What to avoid
It is best to stick to soft, cool foods while you recover from wisdom teeth removal surgery. Try and avoid spicy foods that can cause pain and irritation in the mouth, as well as crunchy foods that can get stuck in your wounds. Stay away from foods that require a lot of chewing while you heal.
If you are concerned about your wisdom teeth and would to make an appointment to see us, please get in touch with us here. We offer a range of oral surgeries at our practice in Melbourne. For a full list of the procedures that we offer, please have a look here.